Synonyms.—Ague; Chills and Fever; Intermittent Fever; Swamp Fever; Marsh Fever; Paludal Fever.
Definition.—A specific, infectious, although non-contagious fever, caused by the hematozoa of Laveran, and consisting of two distinct parts: First, a succession of exacerbations and intermissions, or a series of short fevers separated by short intervals of health; second, a continued fever made up of exacerbations and remissions, there being but one cold stage. The disease is characterized by congestion of the spleen and portal circulation.
History.—Although Rome, secure on her seven hills, had conquered and ruled the world, there was one insidious foe whom she could not overcome. Intrenched in the Pontine Marshes there lurked an enemy that overcame her bravest sons and fairest daughters, and this same formidable foe has been found endemically and occasionally epidemically, from time immemorial, in nearly every clime save the extremes of latitude. During the last fifty years it has been progressively decreasing, and sections where once the disease prevailed in force are now almost immune.
It is more prevalent in the tropics, and diminishes as we recede from them. In Europe, Russia and Italy are the chief points of infection, while Germany, France, and England are rarely visited by the disease. It is also severe in Africa and India. In the United States it prevails largely in the South, while the East, North, and West are but slightly affected. Even in the South, however, there is a marked decrease in the number of cases during the last twenty years.
Etiology.—Soil.—The condition of the soil has been recognized as a causal factor for a great many years by a majority of the profession. A humid soil, producing a luxurious vegetation, was long regarded as a habitat for malaria; and marsh miasm, arising from the decomposition of vegetable matter, was long credited as the principal factor in giving rise to this class of fevers.
That low, marshy, and swampy lands are the great breeding places of malaria has also been recognized from time immemorial. The Pontine Marshes about Rome, a veritable hotbed for the disease, is one of many examples. Fresh-water marshes, situated near the sea, when slightly influenced by salt water, are especially favorable for the generation and multiplication of the parasite or poison.
The specific cause, then, may be said to reside in the soil made rich by the decomposition of vegetable matter, or upon its surface. The exposing of virgin soil, either in the overturning for agricultural purposes, or in digging trenches, or in excavations, has exposed the germs, and epidemics have followed where before the disease was unknown. In contrast to this, malaria has been found to exist in dry, sandy soil, although, in all probability, the poison had been carried by prevailing winds, rather than that such soils are the natural habitat of the disease germs.
Heat.—A temperature of sixty-five degrees is necessary for the development of the hematozoa, and consequently we find the disease prevailing to a far greater extent in the tropics than in the temperate zone. In fact, as we recede from the tropics, there is a progressive decrease in malaria.
Moisture.—A certain amount of moisture seems necessary for the development of the poison, although the large number of cases following a hot, dry summer, seemingly contradicts this statement.
In the tropics the disease prevails to a far greater extent during the rainy season, and the disappearance of malaria by draining marshy sections confirms this view.
Winds.—That the poison may be transferred some distance by strong, winds has been clearly proven by sailors contracting the disease while anchored three to five miles off malarial shores; on the other hand, these same winds, by rapidly drying the soil, may combat its influence.
Trees.—The Eucalyptus-tree at one time was supposed to possess some virtue in combating the toxin, and the marked decrease in large areas where these trees were planted, notably in the Roman Campagna, were cited as proof; but the more rational view is that by drawing large quantities of water from the soil, it was thus rendered sterile to the germ, and that any rapid-growing trees would give like results.
Altitude.—That gravity influenced the poison was very early recognized by people settling in malarial sections, for it was soon learned that by building their houses on high lands they rendered themselves comparatively free from the disease, and that those residing in the second stories of buildings were also largely exempt, while those on the ground floor suffered. The poison is found near the ground, save when carried to higher altitudes by high winds.
Season.—Heat being an important factor in the development of the poison or germ, we find the disease prevailing more extensively in the fall, following the hot weather of July and August, the maximum number of cases occurring in September. While this is true of the temperate and sub-tropical zones, in the tropics as many cases occur in the spring as in the fall.
The Malarial Germ or Parasite.—In 1879, Klebs and Tomassi Crudeli discovered that certain soils, when the conditions of moisture and heat were favorable, resulted in the development of malaria, and they succeeded in isolating a specific germ, which they termed the bacillus malaria, and claimed that it was the specific agent causing all forms of malaria. Other observers, however, after most careful and painstaking study, failed to confirm the claims of these two workers, and it remained for a French army surgeon, Lavaran, in the following year, 1880, to discover in the blood of malarial patients the specific parasite that is now recognized by the medical world as the causal agent in all forms of malaria.
For three years his discoveries and publications caused but little interest in the medical world, but Richard, in 1882, and Marchiafava, Golgi, and Celli in 1883, Italian observers, published their investigations, ratifying the observations of Lavaran. Since then Concilman, Osier, James, Dock, and others of the United States; Van Dyke Carter, of India, as well as French, German, English, and Russian observers, all unite in their declaration that Lavaran's observations were correct, and that the parasite described by him is the specific cause of malaria.
Parasites.—These micro-organisms belong to the hematozoa, a sub-class of the protozoa. Three varieties have been carefully studied, each of which gives rise to a certain kind of malaria. These three are the Tertian, Quartan, and Estivo-Autumnal, other types being simply a development of two or more of these groups at different intervals. These parasites enter the blood corpuscles as minute hyaline bodies, possessing ameboid movement. Having gained entrance into a corpuscle, the further development is at the expense of its contents, converting the hemoglobin into pigment granules, which collect near the center of the parasite. On reaching maturity, segmentation or sporulation takes place, and the membrane or wall of the corpuscles gives way, liberating a fresh generation of hematozoa. They consist of very minute, spherical hyaline bodies, and those escaping the phagocytes enter other corpuscles, and there the process is repeated over and over again.
While the tertian and quartan parasites are thus developed, Golgi's investigations go to prove that the evolution of the estivo-autumnal germs takes place in the spleen, liver, and bone marrow. The evolution of each of these parasites is somewhat different.
Tertian.—The life cycle of this variety is forty-eight hours, sporulation taking place, accompanied by a paroxysm, every third day. The parasite is first seen in the corpuscle as a minute hyaline, ameboid body. It develops at the expense of the red corpuscle, converting the hemoglobin into pigment granules, which range themselves in the center of the parasite. During this process, the blood corpuscles become pale and somewhat increased in size. When completely developed, segmentation or sporulation occurs, and from fifteen to twenty new bodies are formed. At this stage the paroxysm of the fever occurs.
Quartan.—The life cycle of this parasite, or its period of development, is seventy-two hours, the paroxysms occurring every fourth day. When first seen in the blood corpuscles, it is a simple hyaline body resembling the tertian type, although of less size (about one-half the size of the red corpuscle), slower in its development, and occupying more time for its complete evolution.
The pigment granules, dark-brown in color, are coarser than those of the tertian; as they develop, the corpuscle shrinks about the parasite and assumes a brassy color. Having reached its maturity, sporulation or segmentation takes place, and from six to twelve germs are liberated with the rupture of the corpuscular membrane. About this time the paroxysm of the fever takes place.
Estivo-Autumnal.—This is the most irregular of the malarial parasites. At first it resembles those of the tertian and quartan; viz., small, spherical, hyaline, ameboid bodies that require from twenty-four to forty-eight hours for their full development. They have a peculiar and distinct faculty of producing crescent-shaped bodies from the round parasites; these are not seen till after the fever has progressed for several days. The young parasites are seen in the peripheral circulation in their early stages, their further development and segmentation taking place in the spleen, liver, and bone-marrow.
If blood from the spleen be examined, they will be seen in different stages of their evolution. This parasite is much smaller than either of the other forms already considered, has fewer pigment granules, and in sporulation throws off fewer offspring. The blood corpuscle shrinks about the parasite, becoming brassy in color. The irregularity of their development accounts for the different phases of autumnal fever.
Each variety of parasites may develop flagella, which may become separated and float off among the corpuscles. Their exact nature has not yet been determined. From these three forms the different forms of malarial fever are developed,—the quotidian form, from two groups of the tertian, developed on successive days; and this combination of two or more varieties, or two or more groups of the same variety, explains the popular types occasionally seen.
Method of Infection.—There are three theories of the manner in which the parasites enter the system: I. The Water theory; 2. The Air theory; 3. The Inoculation theory.
Water Theory.—A great many examples are cited by Lavaran, Sternberg, and other observers, to prove that infection may take place through drinking water. Three principal experiments will suffice in support of this theory. First, in special malarial sections, where the inhabitants were using water from stagnant pools and suffering from malaria, the disease was made to disappear by furnishing a pure water-supply. Second, malaria introduced into healthy places by using drinking water brought from malarial sections. Third, examples were given where travelers who were passing through malarial countries, preserved their health by using only boiled water, while those of the party who did not take this precaution were attacked in large numbers. While many of the experiments to prove the water theory are plausible, they are not above criticism from a scientific standpoint.
Air Theory.—The air theory has fewer apparently conclusive evidences whereby the disease has been contracted from this source than the water theory, and while sailors have contracted malaria while lying at anchor off shore, while the prevailing winds were directly from the malarial districts, yet it is a well-known fact that the sea-breeze which blows in Rome during the summer months does not bring danger, although it passes over all the numerous foci of malaria in the western half of the Campagna and over all the swamps on the coast. Tomassi Crudeli has proved that the malarial germs rise but a short distance from the ground, and hence are not apt to be carried very far by the prevailing winds.
Inoculation Theory.—This theory, that the germs are inoculated into man through the mosquito, is the only one which has, to date, been demonstrated experimentally.
Bignami, who belongs to the Italian school, after much research, came to the conclusion that malaria acted like a disease inoculated through the sting of a mosquito. To prove the truth of his theory experimentally, he caused perfectly healthy men living in a positively non-malarial section to be bitten by mosquitoes transported from a place where malaria prevailed. These experiments were made with great scientific care, and gave positive results. Through the courtesy of William Wood and Co., publishers of the "Twentieth Century Practice of Medicine," I quote Bignami's description of his experiments:
"Experiment No. I.—Sola slept in the room (in which the infected mosquitoes had been liberated) from September 26th to the end of October, 1898. During the latter part of October the patient complained of malaise and headache. On the afternoon of October 31st he had a slight elevation of temperature to 37.2°C. (99°F.) On November 1st, at about three P. M., he was taken with a severe chill, which lasted until five o'clock, the temperature rising rapidly to above 39°C. (102.2°F.) Between nine and ten o'clock a feeling of cold was again experienced. The fever continued all night, falling in the early morning (November 2d) to 38.2°C. (100.8°F.), and rising again that evening to 39.3°C. (102.7°F.) The patient was restless, and complained of very severe headache, but there were no grave symptoms. In the night, about eleven o'clock, he had another chill of short duration. During this night the temperature remained above 39°C. (102.2°F.), and on the morning of November 3d rose above 40.4°C. (104.7°F.), the patient being very restless and complaining of much suffering. The fever broke in the afternoon with a gentle perspiration.
"At a quarter after five in the afternoon a hypodermic injection of 1 gm. (gr. 15) of quinine was given, and repeated in the night. The fever fell, and at eight A. M., on November 4th, the temperature was 36.7°C. (98°F.) The administration of quinine was continued during the following days; the patient continued to have slight elevations of temperature which did not reach 38°C. (100.4°F.), except once on November 6th. From November 7th onward, the patient was entirely without fever, and rapidly regained his appetite and strength.
"An examination of the blood, made with the greatest care on November 2d, gave negative results, no malarial parasites being found. On the morning of November 3d a few young annular parasites, motile and discoid, without pigment and presenting the characteristic appearance of parasites of estival fever, were found at Maccarese were liberated in this room. The subject of the experiment continued to sleep regularly in the room up to December 2d; he entered it at dusk and left it in the morning, passing the day in the general ward. He asserts that he was bitten by the mosquitoes every night, and there were always found in the room numbers of A. clavinger full of blood. Some of the insects died during this time, but on November 29th there were still found about fifty in good condition.
"The first two days of December the patient was indisposed and had a slight elevation of temperature. On December 3d he had a febrile attack, which began with a chill, the temperature rising to a maximum of 39.7°C. (103.5°?.) Similar attacks, each preceded by a chill, were observed on the following days up to December 7th, when 2 gm. (gr. xxx) of quinine were administered. On December 8th and 9th slight elevations of temperature were observed, but after that none. The patient continued to take quinine for a time, and rapidly recovered. The following are the temperature observations in degrees Centigrade from December 3d to 7th:
"December 3d—4 P. M., 39.8°; 6, 39.7°; 8, 39.7°; 10, 37-5°; 12,37.7°.
"December 4th.—Apyrexia up to 6 A. M.; 8, 37.6°; 10, 38°; 12, 38.9°; 2 P. M., 40.2°; 4, 39.5°; 6, 37.5°; 8, 37.6°; 10, 37.7°; 12, 37.8°.
"December 5th.—Apyrexia up to 10 A. M.; 12, 39.5°; 2 P. M., 39.9°; 4, 40.5°; 6, 39.1°; 8, 38.5°; 10, 37.5°.
"December 6th.—Apyrexia from the last entry up to 8 A. M.; 10, 39.3°; 12, 40.5°; 2 P. M., 37.8°; 4, 38.7°; 6, 38°; 8. 37.1°.
"December 7th.—Apyrexia from last entry up to 10 A. M.; 12, 38.7°; 2 P. M., 38.1°; 4, 38.3°; 6, 37.5°; 8, 37.3°.
"The course of the fever was that of a double tertian. From the first febrile paroxysm, tertian parasites were found in the blood, which followed regularly the development in two generations corresponding to the daily attacks of the fever. A fact worthy of consideration is, that from December 6th—that is to say, four days, or, at the most, five, after the beginning of the disease—the patient had in his blood adult parasitic forms capable of further development in the body Anopheles. And, in fact, many individuals of A. clavinger, which had been bitten about eleven o'clock on the morning of this day, were found later to have the middle intestine infested with tertian parasites."
"Experiment No. 4.—A patient suffering from a relapsing estivo-autumnal infection, in whose blood were many crescents and round and flagellated bodies, slept from December 10th to 18th in a room in which had been set free about fifty individuals of A. clavinger brought from Maccarese. The temperature of the room was maintained at from 18° to 22°C. (64.4° to 71.6°F.) Most of the mosquitoes stung the patient and became infected with crescent bodies, and subsequent examination showed in the middle intestine the characteristic forms in process of development. But it was also observed that the mosquitoes remaining in the room at the given temperature during the last days of December did not have in the intestine mature sporozoa with sporozoites, but only growing forms. Evidently at a temperature of from 18° to 22°C. the life cycle of the parasite is completed very slowly. But these same mosquitoes, confined for a few days in an incubator at a temperature of 30°C. (86°F.), were found to contain forms of a later development. There were noted, indeed, in the intestine, typical capsules filled with sporozoites, and also broken and empty capsules, and in the salivary glands were numerous sporozoites.
"When this fact was noted, three mosquitoes of this group were kept in the incubator at 30°C. for two days, and on January 2d they were made to sting a new subject, A. B——, who lent himself knowingly and willingly to the experiment. It is needless to say that this man had never had malarial fever. On January 5th, two of the same mosquitoes were made to sting the same person again, who then had been stung in all five times by three specimens of A. clavinger.
"After this part of the experiment, the three mosquitoes were dissected and examined under the microscope, with the following result:
"A. clavinger. No. 1.—In the intestine were found very many capsules, with sporozoites, and some capsules which had been ruptured and completely emptied of their contents. In the salivary glands were found two infected tubules; in one were seen the cells swollen, of ovoid form, and filled with granules of uniform size. When pressure was made on the preparation, there issued a very large number of sporozoites of typical form, uniform in appearance, and all of equal length; in the other tubule were also seen cells containing filiform sporozoites of characteristic appearance.
"A. clavinger, No. 2.—In the intestine were found very numerous capsules, some still whole and filled with sporozoites; others ruptured and shrunken, containing a granular residuum of a pale yellow color.' In some of these ruptured capsules were seen also brown bodies of variable size and shape, some elongated, others short and deformed. In the salivary glands all the tubules were infected except one or two. In them were seen cells containing typical sporozoites, cells filled with granules similar to those described in the case of A. clavinger No. 1, and cells filled with round hyaline bodies of variable size. In addition there were also found typical filiform sporozoites along the excretory duct of the gland.
"A. clavinger No. 3.—The intestine was filled with mature sporozoa. Many capsules were broken and shrunken, and contained a pale yellow detritus; others contained a large central body of granular aspect, surrounded by a hyaline halo, and without any recognizable structure. These were possibly mature sporozoa in process of degeneration. The salivary glands were not found infected. From the results of this examination we may conclude that of the three specimens of A. clavinger employed, only two had inoculated the patient with malaria.
"On the evening of January 10th the patient had a sense of heat and headache, but the temperature was normal. On January 11th, 12th, and 13th there was no fever, and the patient felt well. On January 14th—that is, after from nine to twelve days of incubation—there was no fever until eight o'clock in the morning, but then the temperature began to rise rapidly and reached 39.5°C. (103.1°F.), at noon. From this time the fever remained continuous up to January 18th. On January 14th, the temperature fluctuated from 39.5° at noon to 37.5° at 4 P. M. At midnight it was 38.9°; at 2 A. M. on the 15th, 39.5°; at 10 A. M. 37.5°. and at noon 40.4°. On the 16th it varied from 37.2° at 6 A. M. to 40.4° at 4 P. M. The extremes on the 17th were 38.2° at 4 A. M. and 40.4° at 4 P. M. The temperature fell to normal at 6 A. M. on the i8th.
"On January 16th a hypodermic injection of hydrochlorate of quinine 2 gm. (gr. xxx) was administered, and this was repeated on the following day. The patient was entirely without fever on January 18th, but he continued to take quinine, and, except for very slight elevations of temperature on the evening's of January 19th and 22d, he had no further trouble. Recovery was perfect and rapid.
"On examination of the blood on the morning of January 15th, there were found scanty estivo-autumnal parasites, with very fine pigment granules at the periphery. On January 16th there were found also plasmodia without pigment and with granules in normal red-blood corpuscles and in brassy bodies. The parasites disappeared after the exhibition of quinine on January 17th. Thus the infection was rapidly cut short, and no crescent bodies were seen.
"We have in this case a typical example of estivo-autumnal infection beginning with a continued fever, as is usual- in this group of malarial affections. The course of the disease was in every respect identical with that in the first case of malarial fever, experimentally induced by the stings of mosquitoes (the Sola case), described by Bignami."
Thus the life cycle of the malarial parasite in mosquitoes has been proven to be similar to the life cycle of the parasite in man, and that mosquitoes may take the parasite from man and inoculate man with it again. The mosquito responsible for this kind of work is the Anopheles clavinger, which may be distinguished from the harmless variety by taking the vertical position while at rest, while the others, the Anopheles culex, are parallel to the surface while at rest.
Pathology.—The morbid changes that are found in malaria are due to the disintegration of the red-blood corpuscles. The destruction of the corpuscles—and they are found in all stages of dissolution—may be due to the action of the parasite, or a toxin resulting from the bacilli or from metabolic changes of which we are still ignorant.
The anemia that attends malaria is thus explained in the rapid destruction of the red-blood disks. The increase of pigment, melanin, in the spleen, liver, kidneys, blood-marrow, and, in fact, in all the viscera, is due to the conversion of the hemoglobin into pigment granules.
 The spleen is enlarged, of a dark slate-color, and more or less friable. In the more severe or chronic forms it becomes enormously enlarged, and is known as ague cake. The liver partakes of the same changes, although the enlargement is not so great. It is of a dark color, and contains pigment granules. The kidneys are somewhat enlarged, are of a dark-red color, and have the characteristic pigment. Pigment granules are also sometimes found in the white corpuscles. Parasites are found in the phagocytes, and occasionally pigment granules. The leukocytes are not increased.
The spleen is enlarged, of a dark slate-color, and more or less friable. In the more severe or chronic forms it becomes enormously enlarged, and is known as ague cake. The liver partakes of the same changes, although the enlargement is not so great. It is of a dark color, and contains pigment granules. The kidneys are somewhat enlarged, are of a dark-red color, and have the characteristic pigment. Pigment granules are also sometimes found in the white corpuscles. Parasites are found in the phagocytes, and occasionally pigment granules. The leukocytes are not increased.
Division.—Etiologically, malaria is divided into Tertian, Quartan, and Estivo-Autumnal; clinically, into Intermittent and Remittent.
The chief characteristic of an intermittent fever is the distinct and periodic or rhythmic recurrence of its exacerbations and intermissions. Each paroxysm embraces the cold, hot, sweating stage, and the intermission, and is termed an interval or revolution.
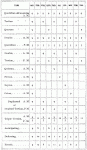 The type of fever has reference to the length of a revolution. Of these there are three principal and two minor. Where the fever makes a revolution in twenty-four hours, it is termed a quotidian type, the fever occurring every day. When it requires forty-eight hours for a revolution, it is termed a tertian type, the fever occurring every third day. Where seventy-two hours are required for a revolution, it is termed a quartan, the fever occurring every fourth day. There may be two revolutions in twenty-four hours, two paroxysms occurring the same day; this is termed a double quotidian; or there may be a recurrence each day, but at different hours, yet each alternate day the paroxysm occurs at the same hour, the fever observing a perfect rhythm; this is termed a double tertian. Other types have been mentioned of long duration, such as quintan, sextan, septan, and octan, although these must be extremely rare, and but few have had the privilege of noticing them.
The type of fever has reference to the length of a revolution. Of these there are three principal and two minor. Where the fever makes a revolution in twenty-four hours, it is termed a quotidian type, the fever occurring every day. When it requires forty-eight hours for a revolution, it is termed a tertian type, the fever occurring every third day. Where seventy-two hours are required for a revolution, it is termed a quartan, the fever occurring every fourth day. There may be two revolutions in twenty-four hours, two paroxysms occurring the same day; this is termed a double quotidian; or there may be a recurrence each day, but at different hours, yet each alternate day the paroxysm occurs at the same hour, the fever observing a perfect rhythm; this is termed a double tertian. Other types have been mentioned of long duration, such as quintan, sextan, septan, and octan, although these must be extremely rare, and but few have had the privilege of noticing them.
There has also been recorded another singular type, where two paroxysms occur one day and none the next, called a duplicated or doubled tertian, or two paroxysms one day and one the next. A fever occurring at an earlier hour each day is called anticipating, while one that occurs at a later hour each day is termed deferring, and one that observes no regular time is termed an erratic type. By reference to the diagram the types may be readily recognized.
Intermittent.—This class may be subdivided, clinically, into simple, inflammatory, gastric, masked, pernicious, and chronic intermittent. The period of incubation depends upon the type of the fever—the tertian about ten days, the quartan ten to fifteen days, the time required for the development of a sufficient number of bacilli or toxin to so forcibly impress the blood as to bring on the paroxysm.
Symptoms.—Incubation.—Although the invasion may be sudden, prodromal symptoms often precede the chill for a few days. They are malaise, languor, listlessness, headache, and a general tired feeling, impaired appetite, and more or less torpor of the excretory organs. The skin is sallow or tawny, and sometimes dry. Each day finds the patient feeling more uncomfortable, till it terminates in a chill.
Cold Stage.—The cold stage varies as to length and character. It may begin with a prolonged rigor, the patient shaking vigorously, his teeth will chatter, and he will be unable to control the convulsive movements; or the invasion may be more gradual; the patient will yawn and stretch, there are chilly sensations that drive him to the fire. There is pain in the head and a general aching of the body. The tongue is dry, with a white coating, and the patient experiences great thirst; the lips are blue, as are also the fingers; the skin is dry and contracted, giving it a roughened appearance, commonly called goose-flesh—Cutis anserina. There is frequently nausea, and sometimes vomiting. The pulse is small but frequent, and the respiration is short and quick. Although the patient feels cold to the touch, if the thermometer be used we will find a temperature ranging from 101° to 103°. This cold stage may last from a few minutes to two or three hours.
Hot Stage.—As the cold stage draws to a close, hot flashes alternate with the chilly sensations, which rapidly increase till all sensations of coldness disappear and the hot stage or period of reaction has full sway. The respiration is full and rapid, the pulse quick and bounding, the face flushed, with throbbing of the carotids; increased pain in the head with restlessness; the tongue is dry and parched, and thirst is constant; the skin is dry and constricted. urine is scanty and high colored, and there is constipation. The temperature may reach 106° or 107°. This stage, like the cold one, may vary as to length of time, from one or two hours to eight or ten hours.
Sweating Stage.—After two or more hours of fever, the temperature begins to fall, the pain in the head ceases, and the sweating stage, or period of excretion, has replaced the former stage. The skin becomes moist, with sometimes profuse perspiration; the secretion from the kidneys is established, is less highly colored, and deposits a sediment. All the unpleasant symptoms disappear, and the patient pronounces himself well.
Intermission.—The stage of excretion is followed by a period of health, of longer or shorter duration, according to the type of the fever. This is followed, in turn, by the cold, hot, and sweating stages, and the fever is made up of these exacerbations and intermissions.
Diagnosis.—The diagnosis is readily made after the fever has made one revolution. The distinct intermission, the temperature becoming normal between the exacerbations, the sallow complexion, the fullness and tenderness of spleen, remove all doubt as to the diagnosis.
Prognosis.—The prognosis is always favorable.
Treatment.—We hear so much of the hematozoa as a cause of malaria, that a large part of the profession takes for granted that an agent which will destroy these micro-organisms will be a specific for the disease. Quinine has been found equal to the test, and the germs disappear upon its administration; hence it is regarded as a specific for intermittents. Yet I am sure that every physician of experience has met cases where this Samson has failed to cure his patient. While quinine is our best anti-periodic and will break the fever, one must know how much to use and when to use it.
The cold stage is usually of short duration and rarely calls for treatment; where long continued, we resort to stimulants externally. The patient may be enveloped in hot blankets, and hot-water bottles applied to the back, sides, and extremities. Internally, ten, twenty, or thirty drops of chloroform administered in syrup may be given every twenty minutes, till reaction is established.
Sedatives.—We now commence our sedatives, aconite and veratrum. In this fever we generally have excess of heart-powder, which is shown by the full, bounding pulse and throbbing of the carotids. With this condition there is great excitation of the nervous system, and we combine gelsemium.
| Veratrum | 20-30 drops |
| Gelsemium | 15 drops |
| Water | 4 ounces. M. |
| Sig. A teaspoonful every one or two hours. | |
These agents shorten and modify the fever, and early establish the secretions, the skin soon becoming moist under the use of veratrum.
Aconite.—If the pulse be small and frequent, aconite replaces the veratrum.
Rhus.—Where there is irritability of the cerebro-spinal centers, as will be shown by the small, hard pulse, restless condition, elevated papilla on tongue, irritability of stomach, we prescribe,—
| Aconite | 5 drops. |
| Rhus | 8 drops. |
| Water | 4 ounces. M. |
| Sig. A teaspoonful every hour. | |
Belladonna.—Where there is marked capillary congestion, which will be shown by the small pulse, the dull expression of face, with dilated pupils, we combine belladonna with our sedative:
| Aconite | 5 drops. |
| Belladonna | 10 drops. |
| Water | 4 ounces. M. |
| Sig. A teaspoonful every hour. | |
These agents not only shorten the fever, but prepare the system for the administration of the antiperiodic during the intermission. Where the temperature is very high, the wet-sheet pack may be used in addition to the sedative.
Quinine.—Success in the use of quinine depends upon the condition of the stomach to absorb it, the amount to be given, and the time of its administration. The tongue must be moist and comparatively clean, or the agent will fail. The amount will be fifteen grains, administered in broken doses, or, if there be time but for a single dose before the expected chill, administer ten grains. I think that the efficiency of quinia is increased by the addition of phosphate of hydrastine. This was a favorite prescription of my father's, and patients came for miles to procure the old yellow powders :
| Quinia | 15 grains. |
| Hydrastine Phosphate | 6 grains. M. |
Divide into three powders, and give one every two or three hours during the intermission, so that the last will come one hour before the expected chill. This may be increased or diminished as the case may require. It may be administered in capsules or solution. I would advise against the use of pills, unless the physician prepares them himself, and knows that they are freshly made. Many pills that are on the market are old and insoluble, and are often passed from the bowels unchanged.
A solution of quinia with syrup of yerba santa makes a quite palatable combination, and where the patient can not swallow a capsule, this is a desirable form. Many like the action of prussiate of iron with quinia as follows:
| Quinia | 15 grains. |
| Prussiate Iron | 10 grains. M. |
| Divide into three powders, and give as above. | |
With a return of a new exacerbation, the sedatives are to be repeated, and with the return of the intermission, we again resort to quinia. Usually, in simple intermittent, the paroxysm is arrested at the end of the second or third revolution. To prevent a return, it is well to continue the quinia, in small doses, for two or three days after the fever is arrested, and every seventh day for three or four weeks.
If there be torpor of the liver and bowels, Podophyllin and leptandrin may be administered; or where there is portal congestion with swelling of spleen, chionanthus and polymnia will prove of great benefit. An inunction of quinia and lard will prove highly beneficial:
| Lard | 2 ounces. |
| Quinia | 1 drachm. M. |
Rub over the abdomen, in the groins and in the axilla, every three or four hours.
Strychnia.—There are some patients who can not take quinia: a very good substitute is strychnia, given hypodermically, 1/30 of a grain one hour before the chill.
Fowler's solution of arsenic is also a good agent where the skin is doughy, tongue small, with a mucoid coating and inclined to a bluish cast:
| Fowler's Solution | 20 drops. |
| Water | 4 ounces. M. |
| Sig. A teaspoonful every hour during the intermission. | |
The Eclectic Practice of Medicine, 1907, was written by Rolla L. Thomas, M. S., M. D.

